The global health lottery
Life’s a literal gamble
A roll of the dice
Where you live shouldn’t determine whether you live. I’d wager that the vast majority of people would agree with that statement. And yet, we live in a world in which it isn’t true. Adding insult to injury, deeply rooted structural systems exacerbate and perpetuate health inequalities, with deadly consequences.
If you’re reading this newsletter, you likely already know that. So let’s dig deeper and quantify and visualise those inequalities. My colleague, Luca Picci, recently dug into the inequitable distribution of healthcare spending. His analysis—and the cool data visualisations he designed—are worth your time.
— Joe Kraus, Senior Director, ONE Data
3 things to know
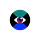
1. A fraction of the world’s health spending goes to low-income countries. High-income countries account for 78% of total health spending. That enables them to fund preventive care, robust health infrastructure, and oftentimes universal coverage. They spend $3,038 per person on average on healthcare. Low-income countries, meanwhile, spend just $45 per person—67 times less.
That spending disparity hits hard: If you live in a high-income country, you stand a good chance of celebrating at least 80 birthdays. The average person living in a low-income country will experience 15 fewer birthdays. That’s roughly 5,500 fewer sunrises, sunsets, and days spent building memories with children, grandchildren, and friends.
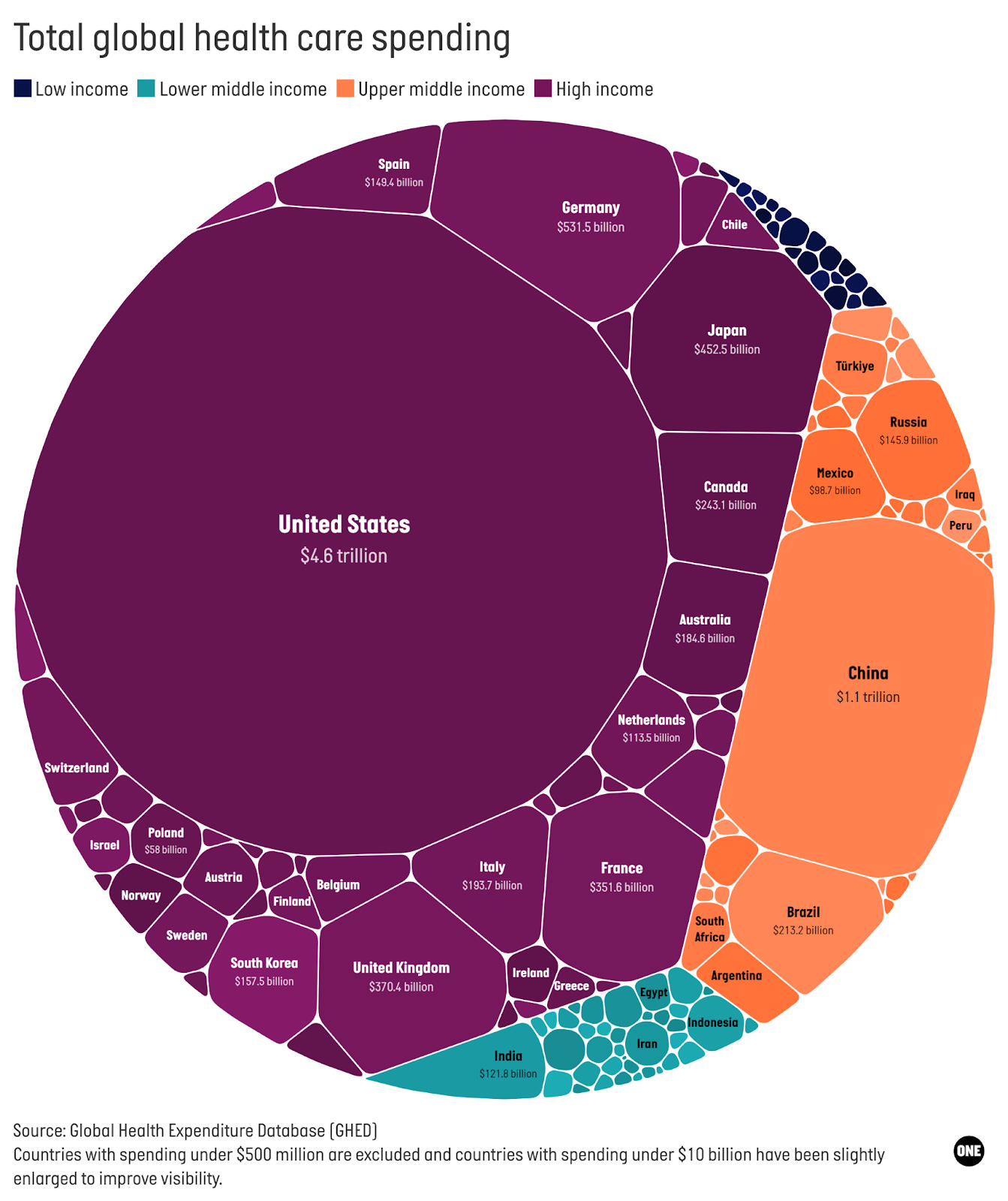
2. People in low-income countries often pick up the healthcare tab. Out-of-pocket payments account for 43% of health spending in low-income countries, compared to around 13% in high-income ones. In 27 countries, out-of-pocket payments account for over half of all health spending. In some countries, like Nigeria, Equatorial Guinea, and Cameroon, over two-thirds of health expenditure is paid out-of-pocket.
That exacerbates inequality: Out-of-pocket spending is one of the most inequitable ways to finance healthcare. Families without resources often deplete savings, sell assets, or cut spending on other essentials like food, education, and housing to cover medical bills. Others avoid treatment altogether, leaving health needs unmet. Sustainable public financing, pooling of resources, and stronger financial protection policies are essential to shift that burden away from individuals and families.
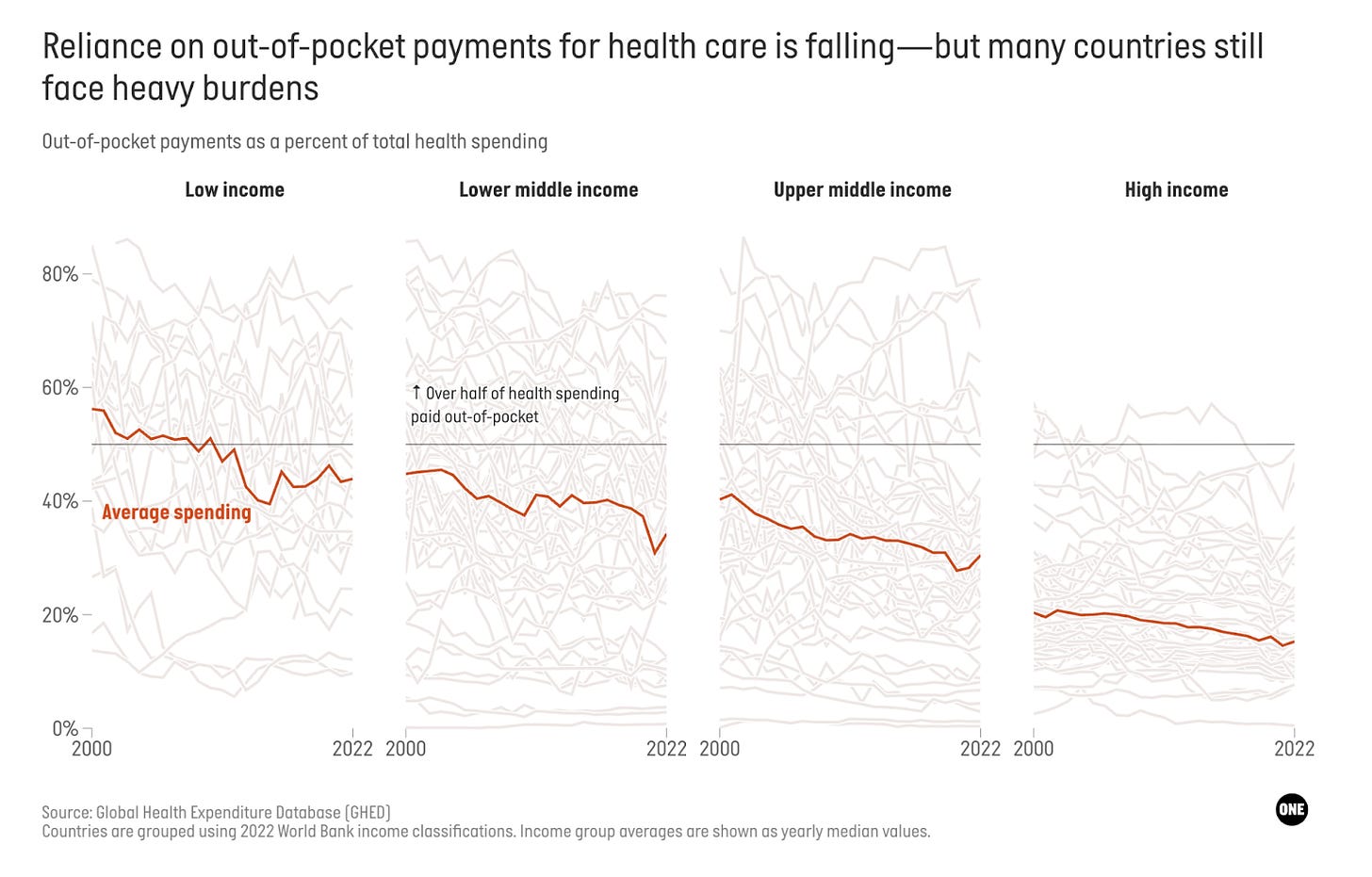
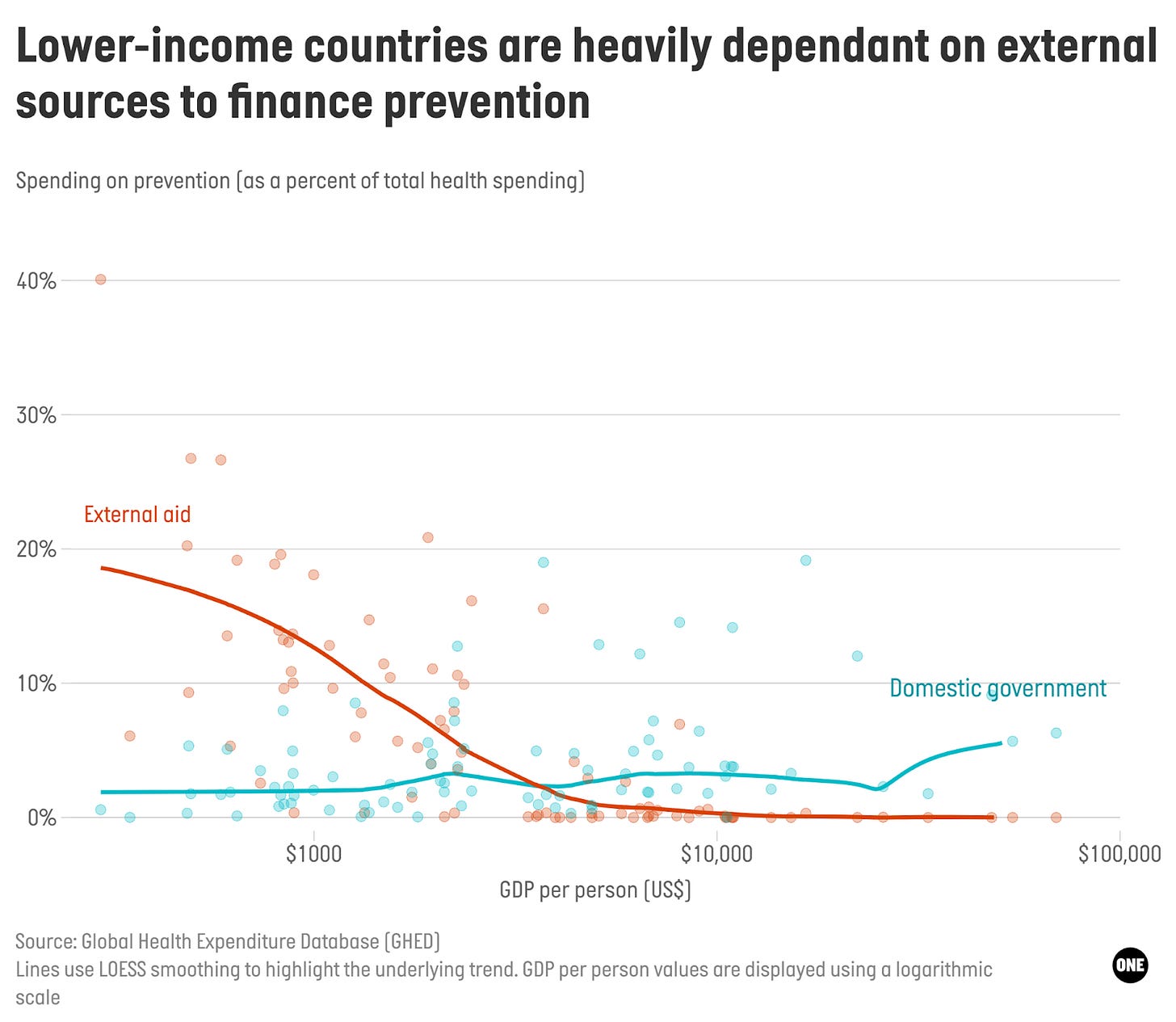
3. Preventative healthcare gets squeezed. Most governments tend to prioritise treating illness and disease over preventing them. Our analysis found a counterintuitive pattern: The share of prevention spending is higher in lower-income countries than in high-income countries. That is something to celebrate, right? Right??
Wrong (sort of): Prevention in lower-income countries is largely financed by external sources. Donor-funded vaccine campaigns, disease control programs, and other preventive initiatives increase the amount spent on prevention. While it’s good that prevention gets funded, the reliance on external financing poses a vulnerability. If (ahem, when) that money dries up, so too does prevention spending.
FROM THE ONE TEAM:
Planning to be at the World Bank & IMF Spring Meetings? Register for our co-hosted event with the AU on translating G20 commitments into concrete action.
ONE’s CEO Ndidi Okonkwo Nwuneli managed to find time in her busy schedule to finish a PhD.
David McNair spoke with the Lead Change podcast about how data can mobilise coalitions for change.
Adrian Lovett spoke to The i Paper about cuts to life-saving support leaving the world more vulnerable to the next pandemic.
IN THE QUEUE:
Nigerians have a Taylor Swift problem.
10 clichés in African governance discourse that need to die.
Make the world safe again.
How the solar boom is playing out in one West African village.
ONE Data provides cutting edge data, tools, and analysis so that we can fight together for a more just world. See for yourself.